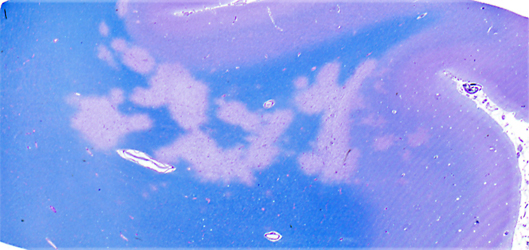
PROGRESSIVE MULTIFOCAL LEUKOENCEPHALOPATHY
Progressive multifocal leukoencephalopathy (PML) is a deadly demyelinative disease of the CNS due to lytic infection of oligodendrocytes by the ubiquitous opportunistic polyoma virus JC(JCV). Most persons acquire this virus at a young age. After primary infection, it remains latent in the kidneys and lymphoid tissues for life. The virus is reactivated and mutates when cellular immunity is severely suppressed. It is not clear how it reaches the brain or why it is neurotropic. It may be latent in the brain from the start or may be brought into the brain by infected leukocytes after it is reactivated. The vast majority of PML cases occur in patients with AIDS. About 10% develop in patients with hematologic malignancies, such as non-Hodgkin lymphoma and chronic lymphocytic leukemia following cytotoxic chemotherapy or irradiation, another 10% in transplant recipients and patients with rheumatologic disorders receiving immunosuppressive therapy and about 5% in MS patients treated with the monoclonal antibody Natalizumab. In classic PML, as it was reported initially there is no inflammatory reaction. Less frequently, some immune reaction is seen. This is most pronounced In PML occurring in the background of the immune reconstitution inflammatory syndrome (PML IRIS) which develops following the initiation of antiretroviral therapy in HIV-infected patients. BK, a member of the same virus family, causes nephropathy in renal allografts, leading to graft loss.
Clinically, PML is characterized by a variety of neurologic deficits (visual loss, paralysis, dementia) evolving rapidly and causing death in a few months. In PML IRIS the symptoms get worse or previously subclinical PML becomes unmasked. PML lesions are located in the subcortical white matter and are hyperintense on T2-weighted and FLAIR sequences. They show no contrast enhancement or mass effect. The CSF is either normal or shows a few lymphocytes. In PML IRIS the lesions show contrast enhancement, edema and mass effect.
Pathologically, PML is characterized by a triad of demyelination, enlarged oligodendrocytes with intranuclear viral particles and bizarre enlarged astrocytes. Demyelination begins with small foci at the cortex-white matter junction. Coalescence of these foci results in large irregular white matter lesions that involve the cerebrum, cerebellum, and brainstem. Myelin is destroyed; axons are relatively spared. PML is a lytic infection leading to oligodendrocyte destruction. The nuclei of infected oligodendroglial cells are packed with viral particles that cause them to enlarge and have a ground glass appearance. Viral particles may also be present in neurons and astrocytes.
Polyoma viruses can also become incorporated into the host genome and cause neoplastic transformation. Such non-lytic infection involves astrocytes and causes pronounced atypia, simulating neoplastic change. Inflammation, other than macrophages, is usually minimal in classic PML. Cases of PML-IRIS have the general pathological features of PML but show brisk inflammation and lack intranuclear inclusions and JCV reactivity by immunohistochemistry. There is no peripheral nerve demyelination or disease in any other organ system. The diagnosis of PML can be made by microscopic examination of a brain biopsy with immunohistochemistry and in situ hybridization for JCV. The diagnosis can also be established with CSF PCR for JCV but this is less sensitive in patients undergoing antiretroviral therapy. In some cases, JCV infects cerebellar granular cells causing cerebellar atrophy and ataxia or cortical neurons causing encephalopathy. Rare cases of aseptic meningitis with JCV present in the CSF but without PML lesions have also been reported.
In addition to its clinical significance, PML is interesting as a model of demyelination due to a lytic infection of myelin-producing cells. Neurotropic mouse hepatitis virus and canine distemper virus are animal models of virus-induced demyelination, similar to PML.
Further Reading
- Koralnik I J. Progressive Multifocal Leukoencephalopathy Revisited: Has the Disease Outgrown its Name? Ann Neurol 2006;60:162-173 PubMed
- Kleinschmidt-Demasters BK, Miravalle A, Schowinsky J, Corboy J, Vollmer T. Update on PML and PML-IRIS Occurring in Multiple Sclerosis Patients Treated With Natalizumab. J Neuropathol Exp Neurol. 2012 Jul;71(7):604-17 PubMed.
- Cortese I, Reich DS, Nath A Progressive multifocal leukoencephalopathy and the spectrum of JC virus-related disease. Nat Rev Neurol 2021 Jan;17(1):37-51. PubMed
Updated: March, 2023