NEURAL TUBE DEFECTS
The neural plate appears on the 17th day of gestation as a thickening of the embryonic ectoderm over the notochord. This neuroectoderm gives rise to the central nervous system. On day 18, the neural plate invaginates along the midline, forming the neural groove with the neural folds on either side. By the end of the third gestational week, the neural folds fuse forming the neural tube. Fusion begins at the hindbrain-cervical junction and the hindbrain-forebrain junction and proceeds rostrally and caudally from these two points. Then, the anterior and posterior ends (neuropores) close, completing the process. The cranial end of the neural tube closes by 24 days and the caudal by 25-26 days. Then, the neural tube is covered dorsally by mesenchyme that forms the vertebral arches and skull. Closure of the vertebral arches is completed at 11 weeks of gestation. Defective closure of the neural tube results in neural tube defects (NTDs). Depending on the point of the defect, NTDs may affect the brain (anencephaly, encephalocele) the spinal cord (spina bifida), or both (craniorachischisis), which is most severe NTD.
The conuss medullaris, cauda equina, and filum terminale develop by a different process from a solid rod of progentor cells, distal to the spinal cord proper. During development also, the spinal column elongates more than the spinal cord, such that spinal cord levels end up higher than their corresponding vertebral levels. Abnormalities of this caudal portion of the spinal structures cause the tethered cord syndrome.
In anencephaly, the brain initially protrudes through a defect in the cranial vault (exencephaly) and is gradually destroyed because of mechanical injury and vascular disruption. Eventually, all that is left is a small, vascular mass of disorganized neural tissue (cerebrovasculosa) mixed with choroid plexus. The eyes evaginate from the forebrain before it is destroyed and are preserved. The cranial vault is either absent or collapses over the base of the skull. Damage of the hypothalamus results in adrenal hypoplasia. Anencephaly is incompatible with survival.
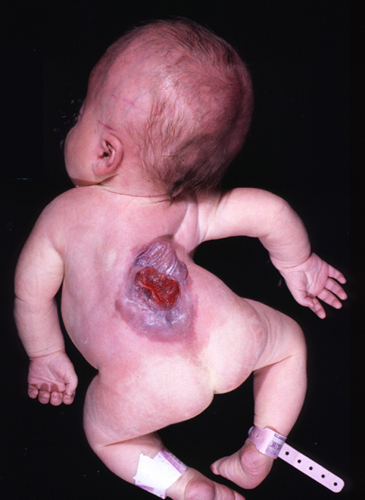
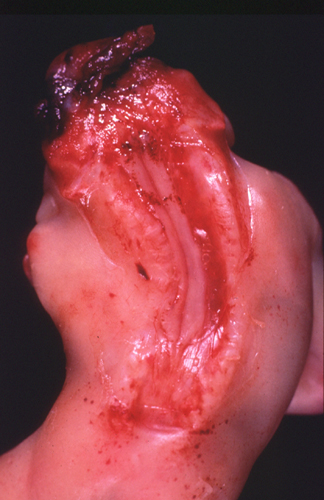
Spina bifida is a set of malformations of the spinal cord caused by failure of closure of the neural tube and lack of fusion of the vertebral arches, soft tissues, and skin that cover the back. The lesion is usually in the lumbosacral area but sometimes it can be more extensive and may involve the entire spinal cord. In its mildest form, spina bifida occulta, the vertebral arches are absent, but there is a hairy patch of skin over the defect. The spinal cord may be normal or the filum terminale may be tethered to subcutaneous tissue. Meningocele is a bulge in the lumbosacral area consisting of a meningeal sac protruding through the bone defect. In meningomyelocele, the sac contains malformed spinal cord tissue. In severe cases, there is no sac at all, and neural tissue from the open neural plate lies on the dorsal surface of the fetus. Anencephaly is often accompanied by spina bifida.
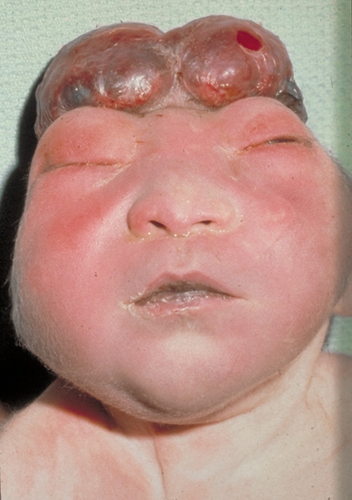
Encephalocele is a protrusion of brain through a defect of the skull, usually in the occipital area. The protruding part is destroyed because of mechanical disruption and ischemia. The intracranial part of the brain around the defect is malformed and disrupted. Large occipital encephaloceles are incompatible with life because of damage of the brainstem.
NTDs are the most common congenital abnormalities of the CNS and, overall, the second most common type of congenital abnormality after congenital heart disease. They are a significant cause of fetal loss. Live-born babies with myelomeningoceles may have paralysis of the legs and loss of bladder and bowel function. Open defects allow entry of bacteria into the CNS. The same thing happens if the skin covering the meningomyelocele becomes necrotic and infected. Some meningomyeloceles are a component of a more complex malformation, the Chiari II malformation, which includes hydrocephalus and abnormalities of the posterior fossa contents (see Chiari malformations further on).
The tethered cord syndrome (TCS) is a frequent accompaniment of meningomyelocele and other malformations of the lower spine and spinal cord. In the TCS, the conus medullaris is pulled lower than the L2 vertebra or the L1-L2 disc space. This traction causes low back pain, scoliosis, lower extremity weakness and sensory loss, and bowel and bladder dysfunction.
Neural tube defects can be detected in utero by determination of alpha-fetoprotein (AFP) and acetylcholinesterase in the amniotic fluid and maternal blood. AFP, a circulating fetal protein produced by the liver, peaks at 12-14 weeks of gestation and subsequently declines. AFP leaks from the fetus into the amniotic fluid through exposed capillaries of the NTD. This results in persistently high levels of AFP in the amniotic fluid and in the maternal blood. Elevated AFP is also seen in other lesions where fetal capillaries are exposed to the amniotic fluid such as omphalocele and sacrococcygeal teratoma. Acetylcholinesterase leaks directly from exposed neural tissue into the amniotic fluid.
NTDs develop during the third to fourth week of gestation and are due to a combination of genetic and environmental causes (multifactorial). The genetic causes are largely unknown. Two polymorphisms of the folate dependent enzyme 5,10-Methylene tetrahydrofolate reductrase (MTHFR), MTHFR C677T and MTHFR A1298C, are associated with an increased risk for NTDs. This enzyme catalyzes the reduction of 5,10-methylenetetrahydrofolate to 5-methyltetrahydrofolate, the active form of folate, which is important for synthesis of nucleic acids and of methionine, which is important for methylation reactions. Administration of 0.4 mg of folic acid in the per siod from 4 weeks before to 8 weeks after conception significantly reduces the occurrence of NTDs. The mechanism of action of folate in preventing NTDs is not known. Women who have children with NTDs are not overtly folate deficient. However, the rapidly dividing cells of the neural tube probably require a large amount of folate for DNA synthesis. Supply of folate may be inadequate because of gene defects that result in subtle abnormalities of folate metabolism. Other causes of NTDs include diabetes mellitus and folate antagonists such as antiepileptic drugs (phenytoin, valproic acid, and carbamazepine).
Further Reading
- Copp AJ, Greene ND. Genetics and development of neural tube defects. J Pathol 2010; 220:217–30. PubMed
- Avagliano L, Massa V, George TM, et al. Overview on neural tube defects: From development to physical characteristics. Birth Defects Res . 2019 Nov 15;111(19):1455-1467.PubMed
Updated: September, 2020